A Closer Look on Closed Comedones and How to Control Them
Have you ever experienced your skin feeling rough, with little bumps that look like whiteheads but not angry-looking enough to be pimples? These bumps are types of acne blemishes called closed comedones; and while they’re not as bad as they look, they may worsen in certain conditions or if they’re not treated properly.
Let’s take a closer look at closed comedones, how they differ from whiteheads and other types of acne, how they are formed, and more importantly, how to treat them and keep them from coming back.
What are closed comedones?
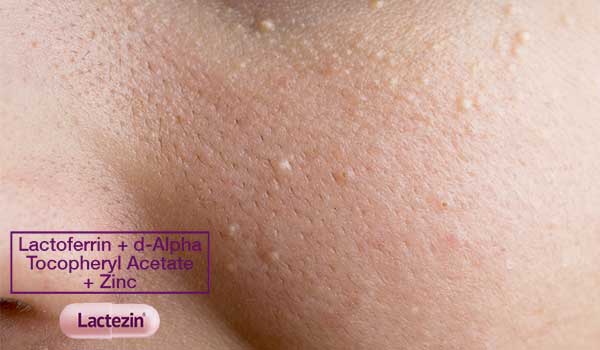
These closed comedones look like tiny, flesh-colored bumps on the skin’s surface. Unlike typical pimples, they don’t appear red and inflamed, and they don’t feel tender or painful.
A closed comedo (singular of comedones) forms when a plug of skin cells and oil becomes trapped within the hair follicle. The plug fills the hair follicle, causing it to swell out and form that bump you see on your skin.
Because closed comedones don’t look like blackheads and regular pimples, they’re often mistaken as whiteheads. Just to differentiate: blackheads are open-faced comedones. When the melanin pigment (found in the sebum produced by your oil glands) comes into contact with air, it oxidizes and turns dark. This process gives blackheads their dark appearance.
On the other hand, whiteheads have closed surfaces and often look like white-colored dots. The reason why closed comedones and whiteheads are mistakenly interchanged is because some closed comedones do develop a white head on the surface. These types of closed comedones are called millia. If the follicle wall around these comedones rupture and get exposed to bacteria, closed comedones can develop into flamed pimples.
Closed comedones can appear anywhere on the skin, but they most often pop up on the face, neck, chest, and back.
What causes closed comedones?
Some individuals, like those with oily skin, are more prone to developing comedones than others. Everyone gets closed comedones at some point in their lives but if you have a lot of them and get them often, you probably have a type of acne called comedonal acne.
Closed comedones are particularly common during teenage years, when fluctuating hormones cause the skin’s sebaceous glands to produce more oil. With all that excess sebum, comedones are very likely to form.
Other contributing factors to comedonal acne include:
- Diet - High dairy consumption, as well as a diet high in fats and sugars, have been linked to comedonal acne.
- Heavy creams and lotions. Closed comedones can form as a result of using products that are occlusive, meaning they essentially seal off the top layer of skin.
- Irritating or oil-based hair products may be behind closed comedones that occur around the hairline or forehead.
- Smoking has also been linked to the occurrence of closed comedones.
- High humidity and air pollution
- Laser therapy or chemical peels
How to treat and prevent closed comedones
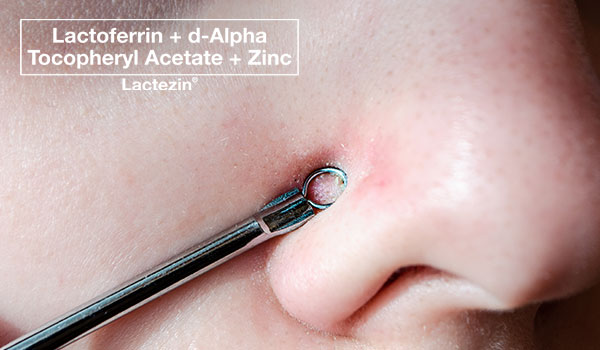
Closed comedones often go away on their own, but this can take weeks or even months. Often, all it takes is a little “push” for these blemishes to turn into pimples. A hormonal surge, an increase in sebum production, a buildup of sweat and bacteria around the already clogged hair follicles, or physical pressure on closed comedones can cause them to reach that inflamed state. So while these small bumps aren’t so bothersome, it’s better to address the problem before it becomes more challenging to treat.
Take note of these tips on how to get rid of closed comedones and prevent them from coming back:
1. Use non comedogenic products.
If you suspect that it’s your products that are causing these bumps, you may want to switch to non comedogenic skincare and cosmetics. Products that are labeled as such are less likely to clog your pores, which means they are less likely to break you out. These products are typically light or water-based, as opposed to heavy and oil-based.
2. Remember to exfoliate gently
By gently, we mean steering clear of harsh, abrasive physical scrubs that can cause microtears on your skin and make things worse. Instead, choose chemical exfoliants that gently break down the bonds between the oil, dirt, and dead skin cells that clog the pores. Look into incorporating AHAs (Alpha Hydroxy Acid) and BHAs (Beta Hydroxy Acid) into your routine. Note: If you’re new to chemical exfoliation, start using these actives at 2% and work your way up once you're sure that your skin can handle it.
3. Apply benzoyl peroxide on affected areas.
Benzoyl peroxide is a classic acne-fighting ingredient that works by eliminating the bacteria that causes pimples and clogs pores. This ingredient is often found on its own in topical acne treatments, but it can also be found in combination with other chemical exfoliants like salicylic acid to make your acne management routine a little more efficient.
4. Consider using medication.
If you have been dealing with a lot of closed comedones, or have been battling them for a while, you may want to see a dermatologist for prescription medication. Your dermatologist may be likely to prescribe topical retinoids, which help clear out existing pore blockages and keep new ones from occurring. These also help smoothen and soften skin. However, you’ll need to be patient to see its full effect: it could take up to three months for a visible change.
Medication with Lactoferrin + d-Alpha Tocopheryl Acetate + Zinc
Another option that may help treat this type of acne is by taking Lactoferrin + d-Alpha Tocopheryl Acetate + Zinc (Lactezin). It is a clinically-tested over-the-counter drug, which uses a natural antibacterial active ingredient Lactoferrin combined with Vitamin E and Zinc to help lessen pimples and give clearer skin in as early as 2 weeks. With continued use, Lactezin may also help keep pimples from coming back.
Lactoferrin + d-Alpha Tocopheryl Acetate + Zinc (Lactezin) is available in all leading drugstores nationwide. You may also purchase online through Lazada and Shopee.
SOURCES:
https://www.aad.org/public/kids/skin/acne-pimples-zits/different-kinds-of-pimples
https://linkinghub.elsevier.com/retrieve/pii/S0190962208009249